Procedures
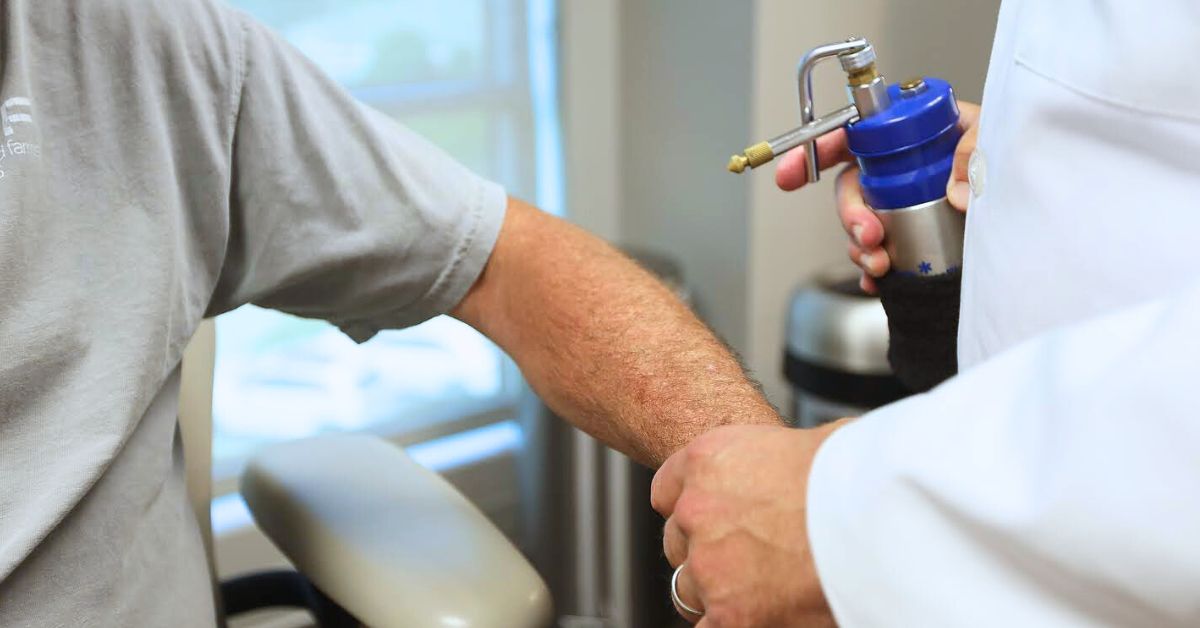
Seborrheic Keratosis Removal Because it’s commonly benign, seborrheic keratosis doesn’t usually require treatment. However, it may be removed for cosmetic reasons, diagnostic purposes, or if it causes discomfort. Read on to learn more about seborrheic keratosis and the most popular methods used for removing it. What is Seborrheic Keratosis? Seborrheic keratosis is a common skin…
Treatments for Skin Cancer Surgical interventions have long dominated the treatment of skin cancer. However, there are also several non-surgical treatments for skin cancer that have developed as the medical world has learned more about this complex condition. Topical Treatments for Skin Cancer Also known as chemotherapy cream, topical treatments for skin cancer are applied…
Surgery for Skin Cancer Skin cancer has layers of complexity that can affect a dermatologist’s approach in terms of diagnosis and treatment. One of the most commonly asked questions about skin cancer treatment is whether or not a patient will require surgery. Although the answer ultimately requires a doctor’s consultation, here are some general guidelines…
Skin Biopsy Procedures Skin cancer affects millions of people globally, as well as countless loved ones and partners who accompany them on their journey. Because of the potentially significant consequences, it is critical that they be addressed swiftly and correctly. To achieve that result, precise skin cancer detection and therapy rely primarily on skin biopsy…